

Contents
Cover
About the Book
About the Author
List of Figures
Title Page
Dedication
Preface to the Second Edition
PART I
YOUR CHILD’S SLEEP
CHAPTER 1: At the End of Your Tether
Can a Child Just Be a ‘Poor Sleeper’?
How to Tell Whether Your Child Has a Sleep Problem
Starting with a Basic Understanding of Sleep
CHAPTER 2: What We Know About Sleep
Non-REM Sleep
REM Sleep
How Sleep Stages Develop in Children
Children’s Sleep Cycles
Sleep and Waking Patterns
The Importance of Biological Rhythms
CHAPTER 3: Helping Your Child to Develop Good Sleep Practices
The Importance of Your Child’s Bedtime Routines
‘Back to Sleep’: Reducing the Risk of SIDS
Should Your Child Sleep in Your Bed?
Specific Issues Related to Co-sleeping
The Sleep Challenges of Multiples: Twins and Triplets
The Special Toy or Favourite Blanket
Developing Good Schedules
PART II
THE SLEEPLESS CHILD
CHAPTER 4: Sleep Associations: A Key Problem
A Typical Sleep Association Problem
Why Sleep Associations Matter
Wrong Sleep Associations
How to Solve the Problem: The Progressive-Waiting Approach
Making the Changes in One Step or Several
Associations to the Breast, Bottle or Dummy
Co-sleeping and Related Considerations
If Things Are Not Getting Better
General Observations
CHAPTER 5: The Problem of Limit-Setting
Who’s in Charge?
Difficulty Setting Limits
Limits, Associations, Feedings, Schedules and Fears
Setting Limits at Night
Limit-Setting Problems: Some Examples
CHAPTER 6: Feedings During the Night: Another Major Cause of Trouble
Is Your Child’s Sleep Problem Caused by Night-time Feedings?
How to Solve the Problem
Other Points to Keep in Mind
Medical Considerations
CHAPTER 7: Night-time Fears
The Anxious Child
Bedtime Fears
Evaluating Your Child’s Fears
How to Cope with Night-time Fears
Techniques to Help a Child Feel Less Frightened and Fall Asleep Quickly
Final Considerations
CHAPTER 8: Colic and Other Medical Causes of Poor Sleep
Colic
Chronic Illness
Nocturnal Pain
Medication
Abnormal Brain Function and a True Inability to Sleep Well
PART III
SCHEDULES AND SLEEP RHYTHM DISTURBANCES
CHAPTER 9: Schedules and Rhythms
Sleep Phases
The Circadian System and the Forbidden Zone for Sleep: Why You Can Stay Awake Until Bedtime – and Sleep Until Morning
Setting the Biological Clock: How Do You Know What Time Zone You Are In?
Individual Differences: Are You a Lark or an Owl?
Society, Sleep Deprivation and the Adolescent
Specific Sleep Problems Affecting Different Parts of the Sleep Cycle: A Summary
CHAPTER 10: Schedule Disorders I: Sleep Phase Problems
Sleep Phases
Sleep Phase Shifts
Sleep Phase Shifts in the Adolescent
CHAPTER 11: Schedule Disorders II: Other Common Schedule Problems
Problems in Regular Schedules
Irregular and Inconsistent Sleep-Wake Schedules
Travel
CHAPTER 12: Naps
Problems with the Length and Timing of Naps
Trouble Giving Up a Nap: Transition Problems
Nap-time Sleep Association Problems
Napping (or Not) at Home and at Day Care
You May Have to Accept What Works
PART IV
INTERRUPTIONS DURING SLEEP
CHAPTER 13: Partial Wakings: Sleep-Talking, Sleepwalking, Confusional Arousals and Sleep Terrors
I. What They Are and Why They Happen
The Normal Transition from Deep (Stage IV) Sleep Towards Waking
More Intense Transitions: A Spectrum of Confusional Events
What a Confusional Event Feels Like
Why Confusional Events Happen: The Balance Between Sleep and Waking
The Variability of Arousals over Time
Evaluating Confusional Events: When to Take Action
II. Treatment
What You Should Do and What Else to Consider
How We Helped the Children Described Earlier
CHAPTER 14: Nightmares
What Nightmares Are and Why They Occur
How to Help Your Child If He Is Having Nightmares
Nightmares and Confusional Events
Nightmares or ‘“No”-mares’?: ‘I had a bad dream’
CHAPTER 15: Bed-wetting
The Impact of Enuresis
What Causes Enuresis?
Approaches to Treating Enuresis
Final Words
CHAPTER 16: Head-Banging, Body-Rocking and Head-Rolling
When Do These Behaviours Occur?
What Do These Behaviours Look Like?
Is Head-Banging Dangerous?
When Should You Be Concerned?
What Causes Rhythmic Behaviours?
Treating the Problem
Outcomes
PART V
THE SLEEPY CHILD
CHAPTER 17: Noisy Breathing, Snoring and Obstructive Sleep Apnoea
What Happens in Sleep Apnoea
What Causes the Obstruction
Treating Sleep Apnoea
Some Words of Caution
Getting Your Child the Help She Needs
CHAPTER 18: Narcolepsy and Other Causes of Sleepiness
Is Your Child Abnormally Sleepy?
Causes of Sleepiness Other Than Narcolepsy
Treating Simpler Causes of Sleepiness
Evaluation at a Sleep Disorders Centre
Narcolepsy
The Cause of Narcolepsy
The Treatment of Narcolepsy
Future Treatments
Index
Acknowledgements
Copyright
About the Author
Dr Richard Ferber is an associate professor of neurology at the Harvard Medical School and the founding director of the Center for Pediatric Sleep Disorders at the Children’s Hospital in Boston. He has over 30 years of experience and has helped millions of families around the world.
About the Book
The proven, gentle approach to help your baby sleep through the night Dr Richard Ferber, the world’s leading paediatric sleep authority, shares his reassuring advice, effective solutions and night-time routines to help your baby, toddler or child get the best night’s sleep.
Help your child:
List of Figures
FIGURE 1 Typical Sleep Requirements in Childhood
FIGURE 2 Brain Wave Patterns in Waking and in Sleep
FIGURE 3 Typical Sleep Stage Progression in the Young Child
FIGURE 4 Helping Your Child Learn to Fall Asleep with the Proper Associations: The Progressive-Waiting Approach
FIGURE 5 Sleep Chart for Parents to Use
FIGURE 6 Betsy’s Sleep Chart
FIGURE 7 Helping Your Child Learn to Stay in His Room
FIGURE 8 Eliminating Extra Feedings at Sleep Times
FIGURE 9 Sleepiness and Alertness Across the Day and Night – Homeostatic and Circadian Drives
FIGURE 10 Common Causes of Sleep Problems at Different Times of the Day and Night
FIGURE 11 Sleep Phase Shifts
FIGURE 12 Too Long in Bed: Potential Sleep Problems
FIGURE 13 Drifting Nap Patterns
FIGURE 14 Spectrum of Behaviour in Children at the End of a Period of Stage IV Sleep
FIGURE 15 Partial Wakings: A Summary of the Major Patterns Across Childhood and General Recommendations for Management
FIGURE 16 Nightmares Versus Sleep Terrors
FIGURE 17 Your Child’s Urinary System
FIGURE 18 Obstructive Sleep Apnoea
FIGURE 19 Use of CPAP
FIGURE 20 How to Tell Whether Your Child Has Sleep Apnoea

To my sons, Matthias and Thaddeus.
As children, they taught me how to be a parent.
As adults, they have taught me to remember being a child.
Preface to the Second Edition
When the first edition of this book appeared in 1985, the medical field devoted to the treatment of sleep disorders in children was new. Still, over the years, the basic information I presented on the nature of sleep and sleep problems in children has remained sound, and the techniques I described to help children with sleep problems have proven to be well conceived and practical. The value of these approaches has been confirmed repeatedly, not only at our sleep disorders centre in Boston, USA, but at many others – and by many different professionals – around the world. Most of the comments I have received from families who carefully read and then applied the techniques outlined in the first edition have expressed gratitude, with parents thanking me for helping them to find a solution to a sleep problem that had been going on for months or years.
So why did I see the need, twenty years later, for this revised and considerably expanded edition? There are three main reasons.
The first reason is to correct some widespread misconceptions regarding my methods and their application. My goals have always been to help parents to understand the nature of sleep and of childhood sleep problems, determine the causes of their own child’s sleep difficulties and choose or design an appropriate treatment programme that fits their own philosophy of child-rearing. I have always believed that the more you understand about your child’s sleep problems, the more humane and effective you can be in solving them. A child may cry repeatedly each night, for example, but until parents understand why that is happening and institute proper treatment, they may be unable to resolve it in a way they find satisfactory.
Despite my efforts in the first edition to communicate these goals, it became clear that they were not always understood as I had intended. Many people thought I recommended a single method to treat all sleep problems, regardless of the nature of the problems, their causes or the parenting styles and wishes of the family. Even worse, the particular method they refer to (only one of many approaches described in this book) has sometimes been incorrectly described as the same ‘cry it out’ method that my suggested techniques were meant to counter. Simply leaving a child in a cot to cry for long periods alone until he falls asleep, no matter how long it takes, is not an approach I approve of. On the contrary, many of the approaches I recommend are designed specifically to avoid unnecessary crying. Most of the sleep problems discussed in this book can be corrected without any crying at all or, if the child is already crying at night, by rapidly reducing it. In the one case where some crying may be necessary – when undesirable nightly practices or habits must be changed – crying can be kept to a minimum.
In this edition I have attempted to make it much clearer that there are many different sleep problems, that apparently identical sleep problems may have different causes in different children and that a single sleep problem may have multiple contributing causes. To properly choose a treatment, one must take all these factors into account. Each problem and cause may require a different treatment (what works well for one problem may be inappropriate for another), and all component causes may have to be treated (a partial solution is no solution at all). In addition, often a number of treatment options are available, some of which fit a particular child’s needs or personality and his or her parents’ desires better than others. I have tried to present more of these choices so that you, the reader, can find an approach you believe appropriate and are comfortable with, whether you live in a big home or small, sleep separately or together or have one child or many; and whether your child is nervous or confident, co-operative or difficult, outgoing or shy.
The second reason for this new edition is to better address topics that were discussed inadequately in the original. Questions from parents have helped me to identify topics that needed to be expanded, such as co-sleeping, naps, sleep problems in twins and travel to different time zones. (The omission of co-sleeping from the original version, apart from a regrettably brief reference that only repeated the conventional attitude of the day, was unfortunate, given the importance of the issue to many parents.) This edition covers such topics in the detail they deserve.
Finally, in this revision I have added new information drawn from the last twenty years’ experience, study and scientific discoveries. We now have more accurate information than we did in 1985 about children’s sleep requirements, and we know more about the biological clock and its effects on sleep and alertness, about sleep terrors and related problems and about medical issues such as bed-wetting, sleep apnoea and narcolepsy. Through my work with thousands of families, I can now offer a number of new methods for treating a variety of common sleep problems.
HOW TO USE THIS BOOK
Sleep problems are rather complex by nature, and to understand and treat them, you need to know a little bit about how sleep works. Although you may be tempted to skip directly to the chapters describing a particular problem of interest to you, I suggest that you begin – regardless of the type of sleep problem you hope to solve – by reading the four general introductory chapters on sleep and sleep rhythms: the three chapters in Part I and Chapter 9, ‘Schedules and Rhythms’ in Part III. These chapters give you the background information you will need to understand most of what appears in other chapters.
You will be best equipped to understand any problem if you also read through most of the remaining chapters. At least skim through them quickly and go back for a closer read once you’ve identified the most relevant material. Many children have more than one sleep problem, and sleep problems are often interconnected. For instance, although the most common cause of sleeplessness in young children – poor sleep associations – is addressed in a single chapter, you may not be able to treat it successfully unless you take into account material from the chapters on limit-setting, fears, schedules or partial wakings. If your child has sleep terrors, you may need to understand the impact of habits and schedules on your child’s symptoms before you can help effectively. And you cannot always deal properly with a problem of limit-setting unless you also take into account your child’s anxiety or an inappropriate bedtime.
Some more specific suggestions follow.
For a sleepless child (including a child who exhibits sleepwalking, sleep terrors or head-banging):
For a child who is sleepy during the day:
For a child who wets the bed:
For a child whose main problem is snoring:
If you base your interventions on the contents of a single chapter and then find that the problems do not resolve quickly, you should stop what you are doing and finish reading the chapters suggested before you proceed any further.
COMMENT ON CASE HISTORIES
As in the first edition, many examples are presented using actual patient histories. Many new ones are included in this edition. Some of the original stories have been retained from the first edition, sometimes with modifications, with some of the names changed to fit contemporary usage. A few of the patients described are composites of several children; however, all descriptions are based on real patients.
Richard Ferber
PART I

YOUR CHILD’S SLEEP
CHAPTER 1

At the End of Your Tether
THE MOST FREQUENT calls I receive at the Center for Pediatric Sleep Disorders at Children’s Hospital Boston, USA, are from parents whose children are sleeping poorly. When the parent on the phone begins by saying, ‘I am at the end of my tether’ or ‘We are at our wits’ end’, I can almost always predict what will be said next.
Typically, the couple or single parent has a young child (often their first) who is between five months and four years old. The child does not fall asleep readily at night or wakes repeatedly during the night, or both. The parents are tired, frustrated and often angry. Their own relationship has become tense, and they are wondering whether there is something inherently wrong with their child and whether they are unfit parents.
In most cases the parents have had lots of advice from friends, relatives and even their paediatrician on how to handle the situation. ‘Let him cry; you’re just spoiling him’, they are told, or ‘That’s just a phase; wait until she outgrows it’. They don’t want to wait, but they are beginning to wonder if they will have to, since despite all their efforts and strategies, the sleep problem persists. Often, the more the parents do to try and solve the problem, the worse it gets. Sooner or later they ask themselves, ‘How long do I let my child cry – all night?’ And if the child gets up four, five or six times a night, ‘Will this phase pass before we collapse from exhaustion?’
Everything seems pretty hopeless at first. If your child isn’t sleeping well or has other problems that worry and frustrate you – such as sleep terrors, bed-wetting, nightmares or loud snoring – it won’t take long for you to feel as if you’re at the end of your tether, too.
Let me assure you that there is hope. With almost all of these children, we are able at least to reduce the sleep disturbance significantly, and usually we can eliminate the problem entirely. The information in this book will help you to identify the type and cause of your child’s particular disturbance, and it will give you a variety of practical ways of solving the problem.
When a family visits the Sleep Center, I meet with the parents and child together and learn all I can about the child’s problem. How often does it arise, and how long has it lasted? What are the episodes like? How do the parents handle the child at bedtime and during the night-time wakings? Is there a family history of sleep problems, and are there social factors that might be contributing to the problem? Given this detailed history, a physical examination and, in certain cases, laboratory study, it is usually possible to identify the disorder and its causes. At that point I can begin to work with the family to help them to solve their child’s sleep problem.
At the Sleep Center, our methods of treatment for the ‘sleepless child’ rarely include medication. Instead, I work with the family to set up new schedules, routines and ways of handling their child. Often the child’s biological rhythms may need normalising, or at least his sleep-wake schedule may need to be changed. He may have to learn to associate new conditions with falling asleep or get used to fewer and smaller night-time feedings. The family may have to learn how to set appropriate limits on the child’s behaviour, and the child may need an incentive to co-operate. And any anxiety in the child (or parent) must be taken into account. I always negotiate the specifics of the plan with the family. It is important that they agree with the approach and feel confident that they will be able to follow through consistently. As much as possible, I offer choices. The best solution frequently differs considerably from family to family, and from one culture or social group to another. If the child is old enough, we include him in the negotiations. Thus, we use a consistent and firm but fair technique tailored to the particular sleep problem and to the needs and desires of the child and family.
Sleep problems are rarely the result of poor parenting. Nor (with a few exceptions) are they part of a ‘normal phase’ that must be waited (and waited, and waited) out. Finally, there is usually nothing physically or mentally wrong with the child himself. Most parents are immensely reassured to know that sleep problems are common in all types of family and social environments and that most children with such problems respond well to treatment.
In certain cases, such as in sleep apnoea or, less often, in bed-wetting, medical factors may be involved, and our intervention may include medication or surgery. Emotional factors may play a role in other instances, such as in the sleepiness of depression, recurrent nightmares in an anxious child, sleep terrors in the adolescent and extreme night-time fears. Here it is important to identify the source of these feelings and to deal with them satisfactorily so the sleep problems can resolve. Sometimes professional counselling is recommended.
How well your child sleeps from the early months affects not only his behaviour during the day but also your feelings about him. I have often heard parents say, ‘He is such a good baby. We even have to wake him for feedings’. Although the parents are really just commenting on the baby’s ability to sleep, they may start thinking that their baby is ‘good’ in the moral sense.
It is easy to see how this distinction can influence the way you relate to your child. If your child does not sleep well, he may well be making your life miserable. It isn’t hard to think of such a child as a ‘bad’ baby. You will probably feel enormously frustrated, helpless, worried and angry if you have to listen to crying every night, get up repeatedly and lose a great deal of your own much-needed sleep. If your child’s sleep disturbance is severe enough, your frustration and fatigue will carry over into your daytime activities, and you are bound to feel increasingly tense with your child, partner, family and friends. If this is the case in your home, you will be pleased to learn that your child is almost certainly capable of sleeping much better than he is now, letting you get a good night’s sleep yourself. To make that happen, you need to learn how to identify your child’s problem; then you can begin to solve it.
The case studies in this book are based on my experience at the Sleep Center. The discussions of these cases, along with descriptions of the underlying sleep disorders and explanations of the methods of solving them, will help you to identify, understand and deal with your own child’s sleep problem.
CAN A CHILD JUST BE A ‘POOR SLEEPER’?
Parents often believe that if their child is a restless sleeper or can’t seem to settle down at night, it’s because he is by nature a poor sleeper or doesn’t need as much sleep as other children of the same age. These beliefs are almost never true. Virtually all children without major medical or neurological disorders have the ability to sleep well. They can go to bed at an appropriate time, fall asleep within minutes and stay asleep until a reasonable hour in the morning. And while it is normal for a child (or an adult) to wake briefly a few times during the night, these arousals should last only a few seconds or minutes and the child should go back to sleep easily on his own.
In fact, the mistaken belief that your child is unable to sleep normally can have a strong influence on how his sleep pattern develops from the day you bring him home from hospital. I have seen many parents who were told by the nurse in the maternity unit, ‘Your baby hardly sleeps at all. You’re in for trouble!’ Because parents like these are led to believe their child is a poor sleeper and there isn’t anything they can do about it, they allow him to develop poor sleep habits; they don’t think it is possible for him to develop good ones. As a result, the whole family suffers terribly. Yet almost all of these children are potentially fine sleepers, and with just a little intervention they can learn to sleep well.
It is true that children differ in their ability to sleep. Some children are excellent sleepers from birth. In the early weeks they may have to be wakened for feedings. As they grow older, not only do they continue to sleep well, but it becomes difficult to wake them even if one tries. They sleep soundly at night in a variety of situations: bright or dark, quiet or noisy, calm or chaotic. They can tolerate an occasional disruption of their sleep schedules, and they sleep well even during periods of emotional stress.
Other children seem inherently more susceptible to having their sleep patterns disrupted. Any change in bedtime routines – an illness, a hospitalisation or the presence of houseguests – can cause their sleep patterns to worsen. Even when these children have always been considered ‘non-sleepers’, we usually find that they, too, can sleep quite satisfactorily once we have made appropriate changes in their routines, schedules, surroundings or interactions within the family. Such children may still have occasional nights of poor sleep, but if the new routines are followed consistently, normal patterns will return quickly.
There are, of course, children who sleep very poorly for reasons we have as yet been unable to identify; however, these problems are extremely uncommon and account for only a tiny percentage of the children we see with difficulty sleeping. For these few, our usual behavioural treatments may help very little or not at all, and medication may even be required. If your child is up a great deal in the night, it may be tempting to assume that he is one of these genuinely poor sleepers. But that is almost certainly not the case. Such instances of truly poor sleep ability are quite rare among otherwise normal young children. In all probability your child’s sleep problem can be solved. He almost certainly has a normal inherent ability to fall asleep and remain asleep. This is true even if he has a sleep disturbance such as sleepwalking or bed-wetting. These problems, occurring during sleep or partial waking, are sometimes bigger management challenges than is sleeplessness, but with the appropriate intervention, they too can usually be decreased significantly if not resolved completely.
HOW TO TELL WHETHER YOUR CHILD HAS A SLEEP PROBLEM
If your child’s sleep patterns cause a problem for you or for him, then he has a sleep problem, whether this problem is just an undesirable expression of normal function or a reflection of an actual underlying emotional or physical ‘disorder’ in the sense of a true psychological disturbance or a physiological abnormality of body function. Sometimes it is easy to see that such a problem exists. Other times sleep problems may be less obvious and easier to miss.
It is usually clear that a problem exists, for example, if your child commonly complains that he can’t fall asleep, or if you find you must be up with him repeatedly during the night. In fact, the most common problems are easy to recognise. They are: frequent difficulty falling asleep at bedtime; waking during the night with an inability to go right back to sleep without parental support or intervention; waking too early or too late in the morning; falling asleep too early or too late in the evening; difficulty getting up for school or day care; and being excessively sleepy during the day. Sleep terrors, sleepwalking and bed-wetting are also readily apparent and quite easy to identify.
Your child could also have a sleep problem that you do not recognise. You may not be able to tell if your child routinely gets too little sleep at night to function normally during the day or if by sleeping late on weekend mornings he decreases his ability to learn during the week. You (and his teacher) may think that when he falls asleep every day in school and on the bus it is because he is bored or unmotivated; in fact, he may not be getting enough sleep, his sleep may be of poor quality or he may even have a disorder, such as narcolepsy, that leaves him unable to stay awake during the day no matter how much sleep he gets and regardless of his motivation. You may see him as lazy or irritable, not recognising that his behaviours are a reflection of poor sleep or of a sleep disorder. You may know he snores loudly every night, but not realise that the snoring is a sign that he might not be breathing satisfactorily, a problem that can interfere with his sleep and leave him overtired and irritable during the day.
It is important to remember that poor sleep affects daytime mood, behaviour and learning. At the same time, you should also know that sleep problems don’t explain all daytime problems. If you don’t know enough about normal sleep patterns, you may fail to recognise sleep problems as the cause of your child’s behavioural or learning difficulties, or you may be tempted to blame these difficulties on poor sleep even when your child’s sleep is perfectly ‘normal’.
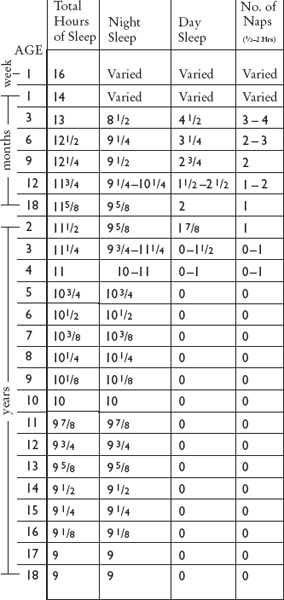
One of the least obvious problems of sleep is simply not getting enough of it. There is no absolute way to judge from numbers alone whether the amount of sleep your child gets per day is appropriate. Figure 1 shows the average amount of sleep children get at various ages during the night and at nap times. Most children will fall within about one hour of the times on that chart. After the very early months, total sleep time per twenty-four-hour period drops to about eleven or twelve hours, diminishing only very gradually after that. The total amount of sleep differs surprisingly little among children, although the way they choose to distribute it may differ. One nine-month-old may sleep nine hours at night and take two solid ninety-minute naps. Another may sleep close to twelve hours at night and nap only briefly during the day.
Children should fall asleep quickly, sleep well at night, wake spontaneously (or at least easily) in the morning and nap only as appropriate for their age. If they do all these things and function well during the daytime, then they are probably getting enough sleep. If it’s always hard to wake them, or if they sleep an extra hour or two on weekends, then they are almost certainly not getting enough sleep. This is especially likely if they also sleep inappropriately (or at least get very sleepy) during the day, or if their behaviour and ability to concentrate deteriorate markedly, typically in the mid-to late afternoon. But each child is different.
We can watch a child’s behaviour during the day closely to see if he seems excessively sleepy or grumpy, but the symptoms of insufficient sleep in a young child can be very subtle. If your two-year-old sleeps only eight hours at night but seems happy and functions well during the day, it is tempting to assume he doesn’t need more sleep. But eight hours is rarely enough sleep for a two-year-old. If you can find out why he sleeps so little and make appropriate changes, he will probably sleep an hour or two longer every night. You may begin to notice an improvement in his general behaviour, and only then will you be aware of the more subtle symptoms of inadequate sleep that were actually present before you adjusted his sleep schedule. Your child will probably be happier in the daytime, a bit less irritable, more able to concentrate at play and less inclined to have tantrums, accidents and arguments.
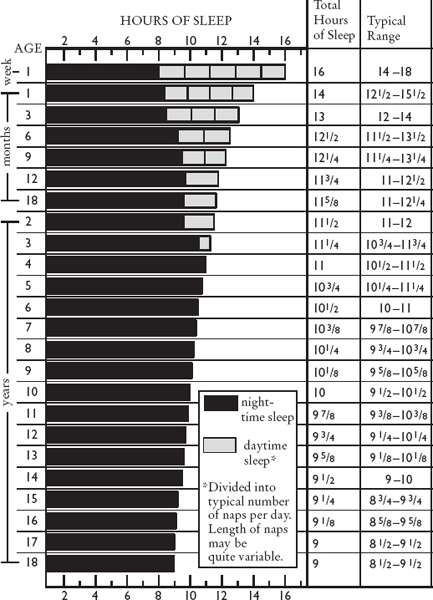
FIGURE 1. TYPICAL SLEEP REQUIREMENTS IN CHILDHOOD
Adolescents almost never get enough sleep. Teenagers are not likely to wake spontaneously on school days, and they almost always sleep late on weekends (at least one hour later than on weekdays and often three to five hours later). When adolescents have the opportunity to sleep as much as they like every night, they average about nine to ten hours per night, and that is probably closer to the optimal level for their age.
Night-time wakings are another potential problem that can be difficult to recognise as ‘abnormal’. A young child (between six months and three years old, say) may be getting adequate amounts of sleep at night even though he wakes several times during the night and has to be helped back to sleep. Parents say to me, ‘Tell me if this is normal. If it is, I will continue getting up; but if it is not, then we would like to do something about it!’ I assure them that most healthy full-term infants are sleeping through the night (which really means that they go back to sleep on their own after normal night-time wakings) by three or four months of age. Certainly by six months, all healthy babies can do so.
If your baby does not start sleeping through the night on his own by five or six months at the latest, or if he begins waking again after weeks or months of sleeping well, then something is interfering with the continuity of his sleep. He should be able to sleep better, and in all likelihood the disruption can be corrected.
STARTING WITH A BASIC UNDERSTANDING OF SLEEP
Before we begin to discuss specific problems and their solutions, you will need some background information about sleep itself, which is covered in Chapter 2. Although you don’t need to be familiar with all the scientific research on sleep, it will be helpful for you to have some understanding of what sleep really is, how normal sleep patterns develop during childhood and what can go wrong. Then you will be better able to recognise abnormal patterns as they begin to develop, to correct problems that have become established and to prevent other problems from occurring.
Although the information on sleep in Chapter 2 is not overly technical, you may be eager to read the later chapters to learn about specific sleep disorders and their treatments. If that is the case, I suggest that you scan the next chapter first and then come back to read it more closely once you have identified your own child’s sleep problem. Most people find the information interesting, and it is especially important for parents who want to help a child sleep better at night.
CHAPTER 2

What We Know About Sleep
ALTHOUGH OUR KNOWLEDGE remains incomplete, a great deal has been discovered about what happens in the brain during sleep: what areas of the brain become active or quiescent, how cellular activity changes and which neurotransmitters (chemicals that carry signals between nerve cells) are released or blocked. Much has also been learned about the so-called biological clock, a small group of cells that keeps our sleep-wake cycle running on about a twenty-four-hour rhythm. This clock controls not only sleep but also variation in just about every other physiological system throughout the day. The cells that constitute it lie in a primitive area of the brain (the hypothalamus) that also controls many other important automatic functions such as hunger, thirst, temperature and hormone levels.
Nevertheless, we do not fully understand why we need to sleep, what causes us to sleep and what purposes sleep serves. There can be no single answer to these questions, in any case, because how you answer them depends on the level at which you approach sleep and waking. At the most basic level, that of neurophysiology, we can say we sleep (and wake) because of changes in the brain’s chemical environment and in its cellular and electrical activity. On a higher level, that of function and behaviour, we can say we sleep because sleep serves a restorative function for our bodies and perhaps our minds. Sleep certainly is necessary for us to function properly during the day: if we don’t get enough of it we feel ‘sleepy’, and this feeling can only be relieved by sleep. Finally, from an evolutionary perspective, the purpose of sleep lies in the benefits it provides for our survival. We can say, as various researchers have, that the purpose of sleep is to protect us from nocturnal predators, to rest the body, to maximise our alertness during the day or to allow us to process memories. If we turn the whole question round and ask, ‘Why do we ever stop sleeping and wake up?’ we could also answer in terms of physiology (because of chemical and electrical changes in the brain) or of function, behaviour and evolution (we need to be awake to eat, procreate and care for our young).
Until the 1950s, doctors and other researchers believed that sleep was a single state distinguishable only from waking. However, we now know that sleep itself is divided into two distinctly different states: REM (pronounced as a single word, ‘rem’), or ‘rapid-eye-movement’ sleep, and non-REM sleep. During non-REM sleep you lie quietly, with a regular heart rate and breathing pattern; it is probably closest to what we usually think of as ‘sleep’, and it provides most of sleep’s restorative properties. There is very little dreaming in this state, if any, although thought-like processes may continue. In REM sleep physiological systems are much more active, and it is in this state that we do nearly all of our dreaming. During the night you cycle back and forth between periods of non-REM and REM sleep as well as having the (usually brief) occasional waking.
NON-REM SLEEP
After the earliest months of life, non-REM sleep divides further into four distinct stages. These stages range progressively from drowsiness to very deep sleep, and they can be identified in the laboratory by monitoring brain waves, eye movements and muscle tone.
As you begin to fall asleep, you enter Stage I, the state of drowsiness. Although you are unaware of it, your eyes move about slowly under your closed eyelids. Your awareness of the external world begins to diminish as well. You have no doubt had the experience of becoming drowsy in a lecture or meeting. As you nod off, you miss some of the speaker’s comments, yet you will jerk awake instantly if your name is called or if your head bends so far forward that you are about to fall off the chair. You might think you hadn’t been asleep at all if it weren’t for your lapse of awareness. On waking from this drowsy state, you might remember some thoughts of the kind usually described as ‘daydreams.’ Some people report seeing or hearing things more like the true dreams that occur during REM sleep, except that they are shorter, less well formed and less bizarre.
If you allow yourself to continue the transition through drowsiness toward deeper sleep, you may notice a sudden jerk of your whole body that actually wakes you briefly and interrupts your descent into sleep. This ‘hypnagogic startle’ is quite normal, although it does not happen every time we fall asleep.
Drowsiness really represents a transitional state between wakefulness and the more fully established stages of non-REM sleep, but we can only identify the arrival of the next stages for certain if we monitor the brain’s electrical activity or ‘brain waves’. At the onset of Stage II, short bursts of very rapid activity (called ‘sleep spindles’) and large, slow waves (‘K-complexes’) begin to appear (see Figure 2). You can still be awakened easily from this stage, but you may not believe that you had really been asleep, depending on how long you had been in Stage II, how deep into this stage you were at the time of waking and, as always, on variations between individuals. As in a waking from Stage I, you would probably not report any odd dream images, but you might describe some thoughts or daydreams.
As you fall into still deeper sleep, you enter Stage III and finally Stage IV (similar stages that together can be thought of as your deep sleep). The smaller and faster brain waves of waking and light sleep disappear, replaced predominantly by large, slow ‘delta’ waves. Your breathing and heart rate become very regular, you may sweat profusely and you will be very difficult to wake. Someone calling your name will no longer easily rouse you, as they would from Stage II sleep; instead, you may be oblivious to the sound.
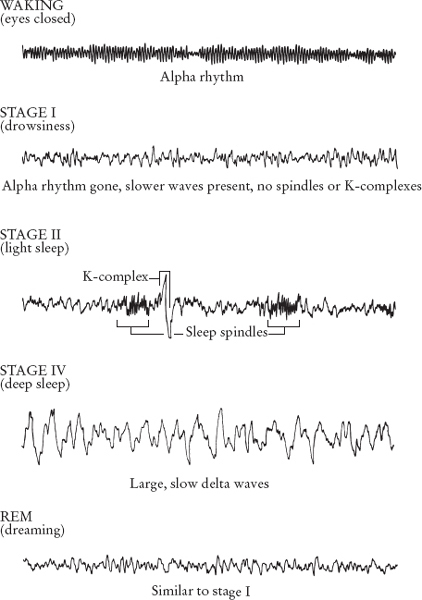
FIGURE 2. BRAIN WAVE PATTERNS IN WAKING AND IN SLEEP
However, if a stimulus is important enough, you will likely wake even from Stage IV. Apparently, even in the deepest sleep our minds can still process some outside information. For example, although it may be difficult to wake you when it is your turn to get up and feed the baby, shouts of ‘Fire!’ or a child’s screams of pain will rouse you promptly. Yet even though you will wake in these emergencies, you will initially be confused. You may be aware that you need to take quick action, but you will have trouble ‘clearing the cobwebs’ from your head so that you can think clearly and sort out what to do. The difficulty one has making the transition from Stage IV sleep to alert waking is very significant in several sleep disorders in children, as you will learn when we discuss sleep terrors, confusional arousals and sleepwalking (Chapter 13).
In non-REM sleep your muscles are more relaxed than when you are awake. You are able to move (unlike in REM sleep, as we will see), but you lie still because your brain is not sending movement signals to most of your muscles. Disorders such as sleepwalking and sleep-associated head-banging are exceptions to this rule.
REM SLEEP
After one or two periods of non-REM sleep you cycle into REM sleep, a different state entirely. Breathing and heart rate become irregular. Your reflexes, kidney function and patterns of hormone release change. Your body’s temperature regulation systems are impaired, so you do not sweat or shiver. Males have penile erections in this state; females undergo clitoral engorgement and an increase in vaginal blood flow. The significance of these genital changes is not known.
REM sleep is an active state. Your body uses more oxygen than it does in non-REM sleep, a sign that you are expending more energy. More blood flows to your brain, your brain’s temperature increases and your brain waves become busy again, resembling a mixture of waking and drowsy patterns. The mind now ‘wakes up’, but the wakefulness of the dream state is quite unlike that of true waking: you respond mainly to signals originating within your own body instead of those coming from the world about you, and you accept without question the bizarre nature of your dreams.
In this state your muscles have very poor tone, especially in the head and neck, and you become profoundly relaxed. Most nerve impulses that would otherwise pass down the spinal cord and out to the muscles are blocked within the spinal cord, so that not only are your muscles relaxed but much of your body is effectively paralysed: signals to move may still be sent out from your brain, but they do not reach your muscles. Only the muscles controlling eye movements, respiration and hearing are spared. Because this blockade is not complete, some of the stronger signals still get through to the muscles, causing frequent small twitches of the hands, legs or face. So although REM sleep is very active in terms of metabolic and brain function, you remain fairly still.
(In babies, the blockade of motor impulses is not fully developed: more impulses get through to the muscles than in an older child or adult. As a result, a young infant in REM sleep will jerk, grimace, twitch, kick and even make sounds. Of course, a newborn cannot get up, walk around and get into trouble. The inhibitory system and the baby mature together, so that by six to twelve months of age – that is, by the time the baby can crawl or walk – most motor impulses are blocked and she stays safely in place.)
The most striking feature of REM sleep is its characteristic bursts of rapid eye movements. During these bursts, the heart rate, blood pressure, respiratory rate and blood flow to the brain all increase and fluctuate irregularly. If you are awakened during one of these bursts, you will almost certainly report that you were having a dream, and the length of the dream you describe will correspond roughly to the time you had been in that state. Children as young as two have described dreams after such wakings. As for younger children, who lack sufficient language to describe dreams, we cannot know for certain that they do dream or what they dream about. However, since all the other features of REM sleep are in place at birth, it is reasonable to presume that even newborns dream. The first dreams are probably very simple repetitions of daily experiences (sounds, smells, sights); dreams then become more and more complex as higher brain centres and language develop.
We cannot say for sure whether your pattern of eye movements indicates that you were actually ‘watching’ your dream occur. We suspect that this is partly true and that at least some of the muscle-twitching corresponds to the actions taking place in the dream. Fortunately, because only a few of the signals to move actually reach your muscles, you merely twitch a little now and then, rather than getting up and moving about, dangerously acting out a dream. One thing this tells us is that sleepwalking and sleep terrors do not result from dreams or nightmares: such complex body movements simply cannot occur during REM sleep.
Some researchers believe that REM sleep has important psychological functions. Their research suggests that REM dreaming allows us to process daytime emotional experiences and transfer recent memories into longer-term storage. Such theories remain unproven. Certainly dreams have emotional significance, but their ultimate importance to the dreamer remains a mystery. REM sleep must serve some purpose, since we all dream every night – even those of us who think we don’t – and if we are deprived of REM sleep for several nights in a row we compensate by getting more REM sleep than usual the next night. Yet, when people are deprived of most of their REM sleep for long periods of time, as a side effect of medication, for example, they don’t seem to show any major ill effects. (Humans cannot be totally deprived of REM sleep, at least not easily. Such studies have been done in animals; complete elimination of REM sleep led to withering and even death.)
Waking a person from REM sleep can be easy or difficult, depending on how important the waking stimulus is to her and how involved she is in her dream. So the clock-radio may not wake you immediately from a really interesting dream; you may even incorporate something you hear on the radio into your dream. On the other hand, an important stimulus such as a burglar alarm will wake you easily and, unlike someone awakened from Stage IV sleep, you will become alert quickly.
To sum up, we seem to live in three distinct states. In the waking state we are rational and we can take care of ourselves and meet our survival needs. In non-REM sleep the body rests and restores itself while the mind rests. And in REM sleep the mind is again active, but it is not rational and it is ‘disconnected’ from the body; major body movements do not take place even though the brain does send out signals to move.
One theory suggests that over the course of evolution REM sleep developed as an intermediate state between non-REM and waking, in which the mind would ‘wake up’ before being ‘connected’ to the body. An animal in non-REM sleep, lying quiet and still except for soft regular breathing, would be relatively safe from predators, but a sudden waking would leave the animal physically active yet confused and disorientated, and thus vulnerable to attack. An animal that first switched into REM sleep would become more alert, but with its brain still disconnected from its muscles it could not make any movement or sound that might alert a predator. Once it was sufficiently alert, the animal could wake fully; the muscle paralysis would disappear, and it could react appropriately to danger. This capacity to check for danger may still be important to humans. We all tend to wake up briefly after an episode of dreaming, and at that moment we are sensitive to anything amiss in our environment: the smell of smoke, footsteps downstairs or quiet sobbing from the next room. If all seems well, we simply return to sleep, and in the morning we probably won’t remember waking up at all. Young children often cannot return to sleep quickly after these normal arousals because something seems ‘wrong’ to them – in one typical situation, it feels ‘wrong’ that they are alone in their cot instead of in a parent’s arms. This common problem is discussed in detail in Chapter 4.
HOW SLEEP STAGES DEVELOP IN CHILDREN
Sleep patterns begin to develop in babies even before birth. REM sleep appears in the foetus at about six or seven months’ gestation, and non-REM sleep follows a month or so later. In the foetus and infant, REM sleep is referred to as ‘active sleep’ and non-REM as ‘quiet sleep’. By the end of the eighth month of gestation, both states are well established.
In the newborn, active sleep is easy to identify because the baby twitches and breathes irregularly and you can see her eyes dart about under her thin eyelids. Sometimes you may also see her smile briefly. In quiet sleep she breathes deeply and lies very still; occasionally you may see fast sucking motions, and now and then a sudden body jerk or ‘startle’.
Quiet sleep is still somewhat different from the non-REM sleep of older children and adults. For one thing, it is undifferentiated: the division into separate, distinguishable stages comes later. The brain waves in quiet sleep show large slow waves occurring in bursts rather than in a continuous flow. During the first month of life the non-REM brain waves become continuous and startles disappear. By the time a baby is a month old, sleep spindles begin to appear, and over the next month or two we can begin to separate non-REM sleep into lighter and deeper stages. K-complex waves (see Figure 2), characteristic of mature non-REM sleep, do not appear until a baby is about six months old, although precursors appear earlier.